Commissioner Lara Proposes Minimal Oversight, Secrecy of Black-Box Wildfire Insurance Models
Proposed Regulation Will Raise Rates but Will Not Stop Home Insurance Companies’ Market Boycott, Says Consumer Watchdog
Los Angeles, CA – Insurance Commissioner Ricardo Lara’s proposal...
Two Bills Holding Community Oil Drillers Accountable Advance To Appropriations Committee
Sacramento, CA—Assembly Bill 3155 (Friedman), which creates new financial liability for oil producers for harm from community oil drilling, cleared its second policy committee...
Legislation Targeting Maternity Ward Closures Helps Families Seek Answers for Available Local Labor and Delivery Services
San Diego, Simi Valley, Latest to Face Closures
Sacramento, CA – Assemblymember Akilah Weber’s bill, AB 1895 requiring the state to conduct community impact assessments before...
Are Draft AI Regs Too Strong or Too Weak? The CA Privacy Agency Can’t Decide.
Do the regs have a loophole?
KCBS - Los Angeles, CA: California Biobank Stores Every Baby's DNA; Parents Had No Idea
04:26
NBC 7 - San Diego, CA: Bill Aims To Slow Maternity Ward Closures
01:49

KGTV-SD (ABC) - San Diego, CA: Who's To Blame For Recent Spikes In Gas Prices?
02:16

FOX 11- Los Angeles, CA: State Farm dropping policies in these California ZIP codes
04:41
CNN - U.S. Cable: 73 Million Former AT&T Customer Accounts Leaked To The Dark Web
03:12

KTXL-SAC (FOX) - Sacramento, CA: Addressing CA's Insurance Crisis
03:12

KPIX-SF (CBS) - San Francisco, CA: Susan Lieu - A Medical Negligance Story
03:52

KPIX-SF (CBS) - San Francisco, CA: Homeowner Insurance Crisis
03:56

KTVU-SF (FOX) - San Francisco, CA: Home Insurance in California
05:12

KABC-LA (ABC) - Los Angeles, CA: California's Insurance Crisis
02:13

KTVU-SF (FOX) - San Francisco, CA: State Farm to Non-Renew Thousands of Policies
03:44

KCAL News - Los Angeles, CA: New Plan to Stop Exodus of Insurers
03:06

KTVU-SF (FOX) - San Francisco, CA: Using Models To Predict Insurance Rate Hikes
02:52

KXTV-SAC (ABC) - Sacramento, CA: Proposed Insurance Changes
02:31

KBCW 44 Cable 12 - San Francisco, CA: Chevy Camaro Thefts On The Rise
02:37

ABC7 - What's California doing to address the insurance crisis?
03:09

KNBC-LA (NBC) - Los Angeles, CA: New Developments in LADWP Overbilling Scandal
03:46

KTLA-LA (CW) - Los Angeles, CA: Request To Unseal Records In DWP/City Attorney Scandal
00:39

KOVR-SAC (CBS) - Sacramento, CA: Signs Fueling Debate Over Gas Tax
02:24

Consumer Alert: More Deceptive Big Oil Ads Targeting California
01:31

KCRA-SAC (NBC) - Sacramento, CA: Struggle To Get State Records
04:19

Consumer Alert — Insurance Attack
02:05

Spectrum News 1 (San Fernando Valley) - Los Angeles, CA: Insurance Revenue: What You Need To Know
03:46

Consumer Alert: Wall Street using AI
01:48

KFMB-SD (CBS) - San Diego, CA: Insurance Rates Spiking Across The County
04:21

KTVU (FOX) - San Francisco, CA: State Farm Has Been Granted An Average Of 20% Increase In Rate Hikes
02:39
KPIX-SF (CBS) - San Francisco, CA: State Farm Home Insurance Rate Hike
01:57
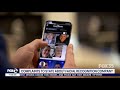
KCBA (FOX) CA: Clearview AI Is Creating An AI Facial Recognition Software That Violates Privacy Laws
00:35

KGO CA: Consumer Watchdog Calls Attorney General to Investigate Clearview AI For Violating State Law
03:06

KGO-SF (ABC) - San Francisco, CA: CRV Fee on Alcohol Starts On January 1st
02:31

KOVR-SAC (CBS) - Sacramento, CA: Car Insurance Cost Rising
02:25
KNTV-SF (NBC) - San Francisco, CA: Tesla Recalls Millions of Cars
02:29

Spectrum News 1 (San Fernando Valley) - Los Angeles, CA: Fire Insurance Affordability
03:52
KGTV-SD (ABC) - San Diego, CA: Doctor Accused of Putting Hidden Camera In A Hospital Restroom
03:22

KGO(ABC)-San Francisco, CA: Consumer Watchdog and the Insurance Commissioner's Office Are In A Brawl
03:12

KABC-LA, CA: Lawmakers Should Prevent Refineries from Selling Expensive Summer Blend of Gas Overseas
02:58

KNBC-LA (NBC) - Los Angeles, CAL: CA To Consider New Rules For Property Insurance Pricing
01:49

KPIX-SF (CBS) - San Francisco, CA: Insurance Overhaul
03:06

NBC Nightly News: Climate Change Driving Up Home Insurance
01:55
KCAL-LA - Los Angeles, CA: Insurance for High Risk Areas
03:02

KTLA-LA (CW) - Los Angeles, CA: Insurance Companies Offering Coverage In CA Fire Zones Again
00:48

KXTV-SAC (ABC) - Sacramento, CA: Changes Coming to Home Insurance Market
02:33

KCBS-LA (CBS) - Los Angeles, CA: CA Insurance Pricing Proposal
02:08

KCRA3 - Sacramento, CA: California Lawmakers to Hold Hearings on Homeowners Insurance Crisis
02:28

KPIX-SF (CBS) - San Francisco, CA: California Gas Prices Are Soaring Again
00:32

KCAL-LA - Los Angeles, CA: Gas Prices Skyrocketing
02:52

KTLA-LA (CW) - Los Angeles, CA: So Cal Gas Prices Nearing $6 a Gallon
03:20

KTVU-SF (FOX) - San Francisco, CA: California Home Insurance Crisis
05:24

KMPH(FOX) - Fresno, CA: Insurance Industry's Focus Will Now Shift to Insurance Commissioner Lara
00:37
In The News
Federal Court Rules Plaintiffs Adequately Alleged CVS Acted With “Deliberate Indifference” When It Adopted Rx Program That Discriminates Against People Living With HIV
Los Angeles, CA – Late yesterday the United States District Court for the Northern District of California ruled that four HIV-positive “John Doe” plaintiffs...
Federal Prosecutors Ordered to Unseal FBI Warrants Related to L.A. City Attorney’s Office and DWP Corruption
Names of Public Officials Including Former City Attorney Mike Feuer Will Not Be Redacted, Nor Will Statements by an FBI Agent that Feuer Lied...
Support Consumer Watchdog
Subscribe to our newsletter
To be updated with all the latest news, press releases and special reports.
